Cervical range of motion norms11/19/2023  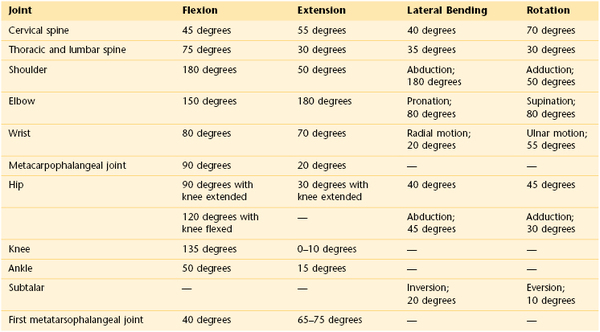
The affected limb should always be compared with the contralateral extremity. If necessary, the examiner can gauge angles by visually dividing a 90-degree arc of motion into two 45-degree segments or three 30-degree segments and projecting the observed angle into these arcs. However, when bony landmarks are not clear because of excess soft tissue coverage or other causes, the goniometer may give inaccurate results. With experience, the orthopaedist may be able to estimate angular measurements accurately, but more reliable measurements are usually obtained with a goniometer. In cubitus varus, the forearm is bent inward toward the midline of the body, distal to the elbow, whereas in coxa vara, the angle between the femoral neck and shaft is smaller than normal and the distal segment is angled toward the midline.Īngular deformities are measured in degrees and are most accurately recorded using a hinged goniometer. Varus describes an angulation toward the midline of the body distal to the anatomic part named (i.e., the distal segment is deviated toward the midline). In coxa valga, the angle between the femoral neck and shaft is greater than normal and the distal segment is angled away from the midline. Approximately 10 to 15 degrees of cubitus valgus, or “carrying angle,” is normal. In cubitus valgus, the forearm is directed away from the midline, distal to the elbow. Valgus denotes an angulation away from the midline of the body distal to the anatomic part named (i.e., the distal segment is deviated away from the midline). The direction of the deformity is designated as either valgus or varus, terms that define alignment in the coronal plane. The specific location of the deformity is denoted by its anatomic name, such as cubitus (elbow, forearm, ulna), coxa (hip), genu (knee), or pes (foot). The description of angular deformities should specify the site of the deformity and the position of the distal segment of the deformity relative to the proximal portion. Is there associated muscle spasm, local tenderness, or pain with motion? Is the deformity fixed, or can it be passively or actively corrected? Is the deformity in the bones, the joints, or the soft tissues? Answers to the following questions will help accomplish this goal: If deformities exist, specific tests can help reveal them. The examiner should look for signs of musculoskeletal deformity, determine what type of deformity exists, and ascertain its exact location. The form used at Texas Scottish Rite Hospital for Children to record the principal findings of the initial orthopaedic examination is provided in Appendix 3-1. Thus the pediatric orthopaedist must not only be familiar with examination of the musculoskeletal system but also knowledgeable about the neurologic examination of the child at different developmental stages. For example, muscle imbalance resulting from cerebral palsy, myelomeningocele, or spinal cord injury may lead to scoliosis or dislocation of the hip joint. Malfunction of the neurologic system can also have a significant impact on the child’s developing skeletal system. The orthopaedist is frequently the first to be consulted for clumsiness or delayed walking in a child, conditions that may be due to static encephalopathy or muscular dystrophy. Because proper function of the musculoskeletal system depends on proper functioning of the neurologic system, the boundary between orthopaedics and neurology is often blurred at the diagnostic level. This chapter covers virtually all aspects of the general musculoskeletal and neuromuscular examination of the neonate, infant, child, and adolescent. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
